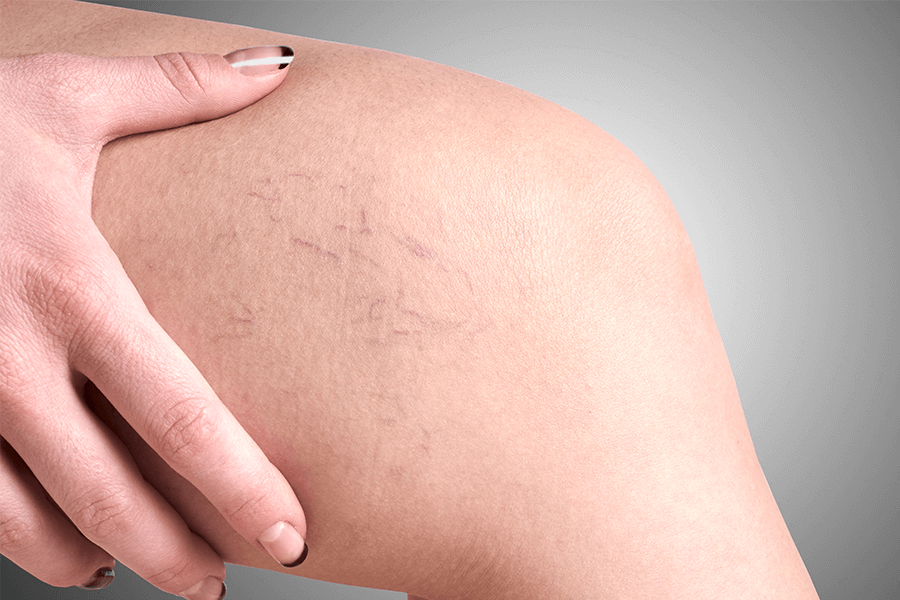
Spider Veins; Causes, Treatment, Prevention
If you have ever noticed a singular or patch of spider veins appear, you may be wondering what caused it, how you can treat it and how you can prevent more from coming! Keep reading to find out. What are spider veins? Spider veins are small, thread-like veins that appear on the skin’s surface and


